Timi risk score early invasive9/3/2023  
In UA/NSTEMI, TIMI scores incorporated the following 7 points: age ≥ 65 years, ≥ three coronary artery disease (CAD) risk factors, known coronary stenosis > 50%, aspirin used in the past 7 days, severe angina (≥ 2 episodes w/in 24 h), severe angina (≥ 2 episodes w/in 24 h) and positive cardiac marker. Risk scoresīoth GRACE and TIMI risk scores were calculated on admission. Briefly, we included NSTEMI patients with acute chest discomfort, elevation of cardiomyocyte necrosis biomarkers, ECG characteristics (transient ST-segment elevation, persistent or transient ST-segment depression, flat or inverted T waves, pseudo-normalization of T waves, or normal ECG). Patients were also excluded if the symptom was caused by severe trauma, medical surgery, or other serious comorbidities. Participants diagnosed with STEMI were excluded. Participants were at least 18 years old, admitted to the hospital with a presumptive ACS diagnosis according to the following points: clinical symptoms, typical ischemic ECG changes, elevated cardiac biomarkers, and documented prior coronary artery diseases. The study population began with 1659 patients consecutively hospitalized with primary diagnose as ACS in the cardiovascular department in Shanghai Renji hospital, China, from Jan 1st, 2017 to Nov 1st, 2017. In this observational study, we sought to (1) examine the distribution of risk tertiles by GRACE versus TIMI in a contemporary cohort of NSTEMI East Asian patients in today's reperfusion era, (2) compare the predictive ability between GRACE and TIMI risk score, (3) explore the optimal way for risk stratification in East Asian population by combining these two scores. Nevertheless, limited evidence compared the usefulness of these two major risk scores and their association with both in-hospital events and long-term outcomes in contemporary East Asian patients. Studies proved TIMI’s advantage in its simplicity in clinical application and GRACE's favorable discriminative power. 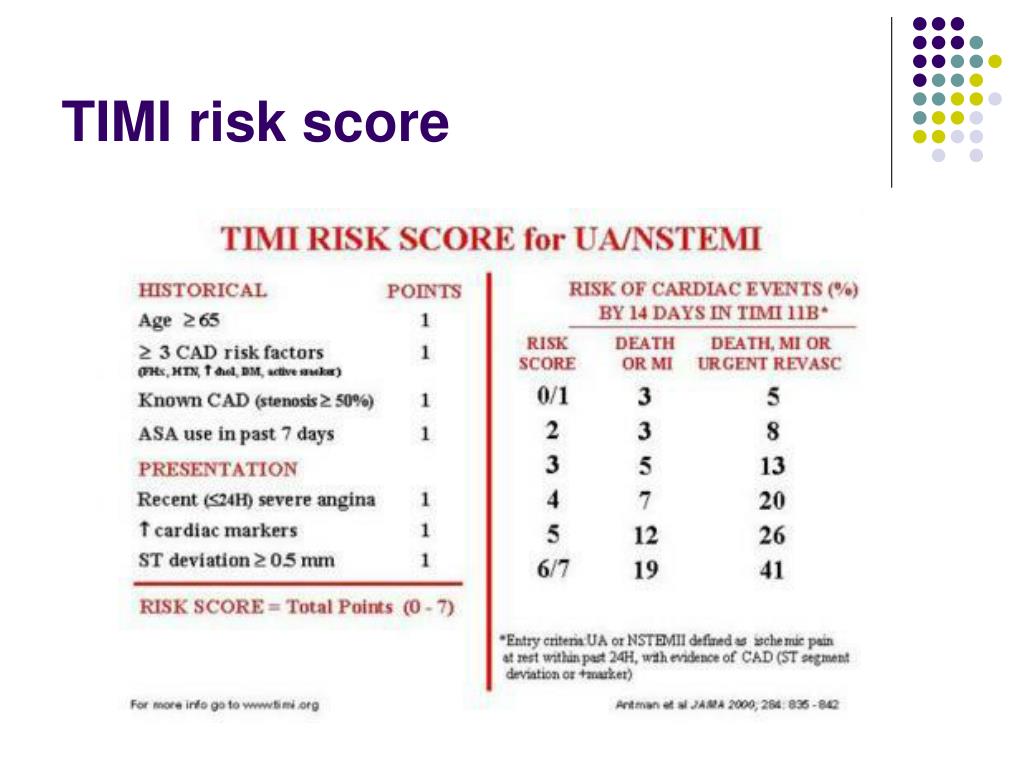
GRACE and TIMI are the two most popular prediction models in ACS developed during the prereperfusion era and have been compared face to face mainly in the Caucasian population. Therefore, there is an essential need to assess individual risk easily and accurately. Guidelines recommend that high-risk patients receive more aggressive invasive treatment upon risk stratification on admission. Risk assessment was crucial in guiding therapeutic decision-making. However, NSTEMI patients have a large range of clinical consequences, from minimal sequelae to early death. A major component of ACS, Non-ST segment elevation myocardial infarction (NSTEMI), has more than twice the incidence compared to ST-segment elevation myocardial infarction (STEMI). The prevalence of acute coronary syndromes (ACS) has increased significantly during the recent 30 years in China. The sequential use of TIMI and GRACE scores provide an easy and promising discriminative tool in predicting outcomes in NSTEMI East Asian patients.Ĭardiovascular disease remains the main contributor to the cause of death globally. GRACE showed better predictive accuracy than TIMI in East Asian NSTEMI patients in both in-hospital and long-term outcomes. Combined use of the two risk scores reserved both the convenience of scoring and the predictive accuracy. 0.68 long-term cardiac mortality: 0.91 vs. GRACE risk scores showed a better predictive ability than TIMI risk scores both for in-hospital and long-term outcomes. Compared to TIMI medium group + GRACE < 140 subgroup, the TIMI medium + GRACE high-risk (≥ 140) subgroup had a significantly higher in-hospital events (39.5% vs. Further subgrouping the TIMI medium group showed that half (53.5%) of the TIMI medium risk population was GRACE high risk (≥ 140). GRACE score grouped most patients (45.7%) into high risk, while TIMI grouped the majority (61.2%) into medium risk. ResultsĪ total of 232 patients were included (female 29.7%, median age 67 years), with a median follow-up of 3.7 years. Long-term outcomes were all-cause mortality and cardiac mortality in 4-year follow-up. In-hospital endpoints were defined as the in-hospital composite event, including mortality, re-infarction, heart failure, stroke, cardiac shock, or resuscitation. Patients were scored by TIMI and GRACE scores on hospital admission. This retrospective observational study consecutively collected patients in a large academic hospital between 01/01 and and followed for 4 years. Limited study compared two risk scores, the Thrombolysis in Myocardial Infarction (TIMI) and Global Registry of Acute Coronary Events (GRACE) risk scores in the current East Asian NSTEMI patients. Risk stratification in non-ST segment elevation myocardial infarction (NSTEMI) determines the intervention time. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
